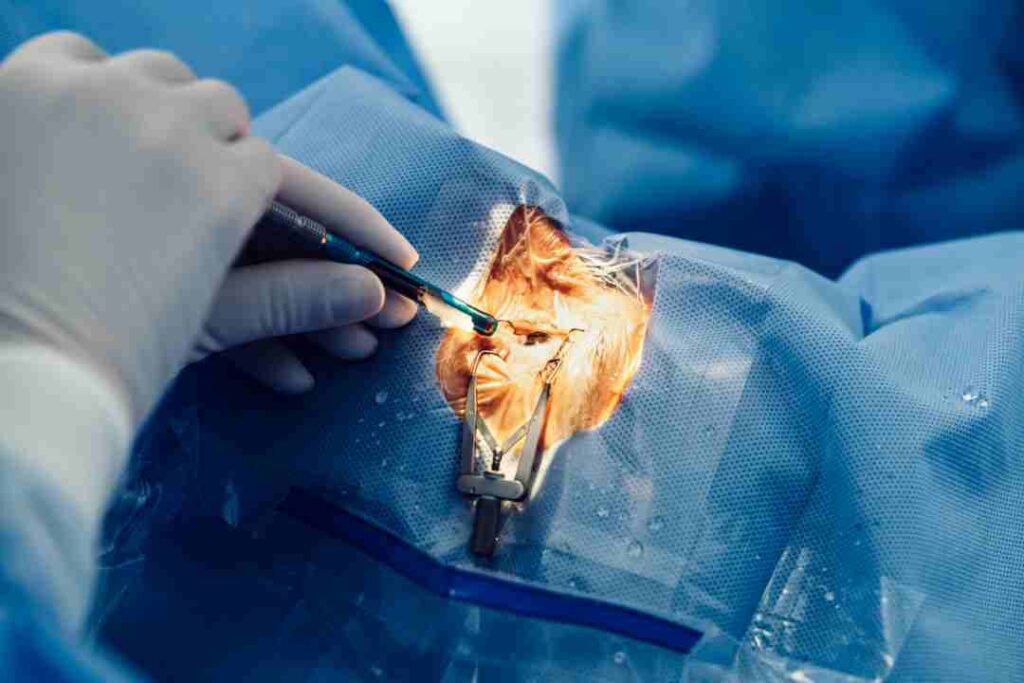
Age-related cataracts are a common eye condition that affects millions of people worldwide. As we age, the lens of our eye becomes less transparent, leading to the formation of cataracts. This article aims to provide a comprehensive understanding of age-related cataracts, including their causes, symptoms, and treatment options.
Understanding Age-Related Cataracts
Cataracts are the clouding of the lens inside the eye, which results in blurry vision and difficulty seeing clearly. Age-related cataracts, as the name suggests, occur as a natural part of the aging process. The lens of the eye gradually becomes less flexible and less transparent, causing vision problems.
What are Age-Related Cataracts?
Age-related cataracts occur when proteins in the lens of the eye clump together, forming a cloudy area. This cloudiness prevents light from passing through the lens properly, leading to blurry vision and other visual disturbances. Age-related cataracts typically develop slowly over time and may affect one or both eyes.
The Anatomy of the Eye and Cataracts
To gain a better understanding of age-related cataracts and their impact on retinal treatments, it’s crucial to familiarize ourselves with the fundamental anatomy of the eye, particularly the part related to retinal health. The eye, a remarkably intricate organ, enables us to perceive the world around us and comprises several distinct components, each playing a unique role.
Among the eye’s critical elements, the lens holds significance. Positioned behind the iris, the colored portion of the eye, the lens is a transparent structure with the primary role of focusing incoming light onto the retina, situated at the eye’s rear. The retina houses specialized photoreceptor cells responsible for converting light into electrical signals, which are subsequently conveyed to the brain via the optic nerve.
In the context of age-related cataracts, which have a direct bearing on retinal treatments, the integrity of the lens is compromised. As cataracts develop, the proteins within the lens begin to aggregate, forming opaque areas that obstruct the unhindered passage of light. Consequently, the light reaching the retina becomes dispersed and distorted, leading to visual blurriness and challenges in achieving clarity of sight.
Age-related cataracts typically progress gradually, often with subtle initial effects on vision. However, as cataracts advance, individuals may encounter mounting difficulties in performing tasks like reading, driving, or recognizing faces. Colors might appear muted or tinged with a yellowish hue, and sensitivity to glare from bright lights may intensify.
It’s important to acknowledge that age-related cataracts are just one category of cataracts, and their interplay with retinal treatments is noteworthy. Other cataract types encompass congenital cataracts (present at birth), traumatic cataracts (resulting from eye injuries), and secondary cataracts (emerging due to other eye conditions or medical interventions).
For those who suspect they have age-related cataracts and are exploring options in the realm of retinal treatments, consulting an eye care professional is a vital step. These specialists can conduct a comprehensive eye examination to assess the extent of cataracts and provide guidance on suitable treatment approaches. In some instances, cataract surgery may be necessary to eliminate the cloudy lens and replace it with an artificial one, thereby restoring clear vision and potentially enhancing the prospects for successful retinal treatments.
Causes of Age-Related Cataracts
While aging is the primary factor in the development of age-related cataracts, there are other contributing factors that may increase the risk of developing this condition.
Age-related cataracts occur when the proteins in the lens of the eye begin to break down and clump together, causing cloudiness and vision impairment. This natural aging process can be influenced by various factors, including genetics and environmental exposures.
Genetic Factors and Age-Related Cataracts
Research suggests that genetics may play a role in the development of cataracts. If you have a family history of age-related cataracts, you may be at a higher risk of developing them yourself. However, it’s essential to understand that genetics alone cannot cause cataracts and that other factors are also involved.
Scientists have identified specific genes that may be associated with an increased susceptibility to cataracts. These genes are involved in the regulation of proteins and antioxidants that protect the lens from damage. Variations in these genes may affect the efficiency of these protective mechanisms, making individuals more prone to cataract formation.
Furthermore, genetic factors can interact with environmental exposures, amplifying the risk of developing cataracts. For example, individuals with certain genetic variations may be more susceptible to the damaging effects of UV radiation or other environmental factors. You can also read about Types of cataracts surgery by visiting https://xraygadgets.com/types-of-cataracts-surgery/
Environmental Factors Contributing to Cataracts
Exposure to certain environmental factors can increase the risk of age-related cataracts. Prolonged exposure to ultraviolet (UV) radiation, such as sunlight or tanning beds, is one of the main environmental factors associated with cataract formation. UV radiation can cause oxidative stress in the lens, leading to the accumulation of damaged proteins and the formation of cataracts.
Smoking is another significant environmental factor that can contribute to cataract development. Cigarette smoke contains harmful chemicals and free radicals that can directly damage the lens and accelerate the breakdown of proteins. Studies have shown that smokers are more likely to develop cataracts at an earlier age compared to non-smokers.
Individuals with diabetes also have an increased risk of developing cataracts. High blood sugar levels can lead to the accumulation of sorbitol, a sugar alcohol, in the lens. This can cause the lens to swell and become cloudy, impairing vision. Additionally, diabetes can weaken the body’s natural defense mechanisms against oxidative stress, further contributing to cataract formation.
Obesity has been identified as a potential risk factor for cataracts as well. Excess body weight and obesity are associated with chronic low-grade inflammation and metabolic imbalances, which can adversely affect the lens and increase the likelihood of cataract development.
Long-term use of corticosteroid medications, such as prednisone, can also increase the risk of cataracts. These medications, commonly prescribed for various inflammatory conditions, can disrupt the balance of proteins in the lens and promote cataract formation.
In conclusion, while aging is the primary cause of age-related cataracts, genetic factors and environmental exposures can contribute to their development. Understanding these factors can help individuals make informed lifestyle choices and take preventive measures to reduce their risk of developing cataracts.
Recognizing the Symptoms of Age-Related Cataracts
Age-related cataracts can cause various visual symptoms that affect daily activities and quality of life. It is important to be aware of these symptoms in order to seek appropriate treatment and support.
Early Signs and Symptoms
In the early stages, age-related cataracts may not cause noticeable symptoms. However, as the condition progresses, common early symptoms may include blurred vision, difficulty seeing in dim or bright light, increased sensitivity to glare, and the need for frequent changes in eyeglass prescriptions.
Blurred vision is a common complaint among individuals with age-related cataracts. This blurriness can make it difficult to read, drive, or perform other daily tasks that require clear vision. It may feel like looking through a foggy window, where objects appear hazy or out of focus.
Difficulty seeing in dim or bright light is another early symptom of cataracts. This can be particularly challenging when transitioning between different lighting conditions, such as going from a well-lit room to a dark hallway. The eyes may struggle to adjust, causing temporary vision impairment.
Increased sensitivity to glare is also commonly experienced by those with age-related cataracts. Glare can be caused by various light sources, such as sunlight, headlights, or even indoor lighting. It can be uncomfortable and make it difficult to see clearly, especially in situations where glare is unavoidable.
Another early symptom is the need for frequent changes in eyeglass prescriptions. As cataracts develop, the eyes undergo changes in their refractive power, leading to fluctuations in vision. This can result in the need for updated prescriptions more frequently than usual.
Progression of Cataract Symptoms
As cataracts progress, symptoms become more pronounced. Individuals may experience double vision in one eye, seeing halos around lights, reduced color vision, and a yellowing or fading of colors. Night vision may also be significantly impaired, impacting driving ability and overall safety.
Double vision, also known as diplopia, can occur when cataracts cause the light entering the eye to scatter, resulting in multiple images. This can be disorienting and make it challenging to navigate the environment effectively.
Seeing halos around lights is another symptom that may develop as cataracts progress. Halos can appear as bright circles or rings around light sources, such as streetlights or lamps. This can cause visual disturbances and make it difficult to focus on objects or read signs accurately.
Reduced color vision is a common complaint among individuals with advanced cataracts. Colors may appear dull or faded, making it challenging to appreciate the vibrancy of the world. This can impact the enjoyment of activities such as art, nature, or even watching television.
Yellowing or fading of colors is another visual change that can occur as cataracts progress. This is often described as a yellow or brown tint that affects the perception of colors. It can be particularly noticeable when looking at white objects, which may appear more yellowish or dingy.
Night vision impairment is a significant concern for individuals with cataracts. The condition can cause difficulty seeing in low-light conditions, such as driving at night. This can lead to increased accidents and a decrease in overall safety. It is important for individuals experiencing this symptom to seek medical attention promptly.
Overall, age-related cataracts can cause a range of symptoms that impact vision and daily life. Recognizing these symptoms is crucial in order to seek appropriate treatment and support. If you or someone you know is experiencing any of these symptoms, it is recommended to consult with an eye care professional for a comprehensive evaluation.
Diagnostic Procedures for Age-Related Cataracts
The diagnosis of age-related cataracts involves a series of comprehensive eye examinations and specialized tests.
Eye Examination Procedures
During an eye examination, an ophthalmologist or optometrist will thoroughly assess the health of your eyes, looking for any signs of cataracts. This examination typically involves testing visual acuity, evaluating eye movements and coordination, and inspecting the structures of the eye using various instruments.
Diagnostic Tests for Cataracts
To confirm the presence of cataracts and determine their severity, additional diagnostic tests may be performed. These tests may include a slit-lamp examination to examine the front part of the eye, a retinal examination to assess the back part of the eye, and measures of contrast sensitivity to evaluate the impact on vision quality.
Treatment Options for Age-Related Cataracts
While there is no proven way to prevent age-related cataracts from developing, several treatment options are available to improve visual function and quality of life.
Non-Surgical Treatment Options
In the early stages of cataract development, non-surgical interventions may help manage symptoms. These include the use of prescription eyeglasses or contact lenses to correct refractive errors, magnifying lenses for reading, and improved lighting conditions to minimize glare and improve visual clarity.
Surgical Treatment Options
If age-related cataracts significantly affect daily activities and visual function, cataract surgery is usually recommended. During this outpatient procedure, the clouded natural lens is removed and replaced with an artificial intraocular lens (IOL). Cataract surgery is considered safe and effective, with minimal risks and a high success rate, improving vision in the vast majority of patients.
In conclusion, age-related cataracts are a common eye condition caused by the natural aging process. While genetics and environmental factors may contribute to their development, age remains the primary risk factor. Recognizing the symptoms and seeking prompt diagnosis and treatment are essential for maintaining visual health and overall well-being. If you suspect age-related cataracts, consult with an eye care professional to explore the appropriate treatment options available to you.